image by flickr.com
My mom told me that she had breast cancer in late 2011. She said that she noticed a red spot on her right breast that was tender to the touch. A few months later, she felt a lump in that same breast. She went to her doctor, who promptly did a mammogram, ultrasound, and biopsy. The ultrasound tech, on the day of the scan, said that she needed immediate surgery to remove the breast and asked if she would like to have both breasts removed just in case. She was stunned. I was not happy for reasons I will talk about later, but let’s discuss mammograms for now.
What Is A Mammogram?
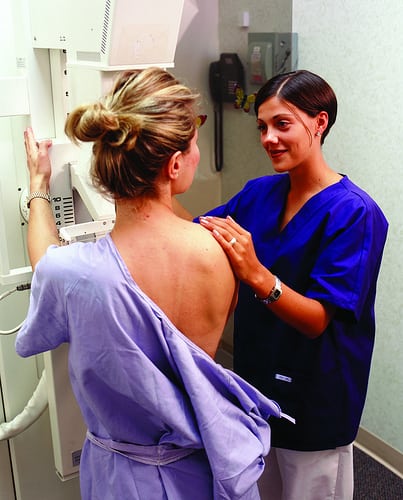
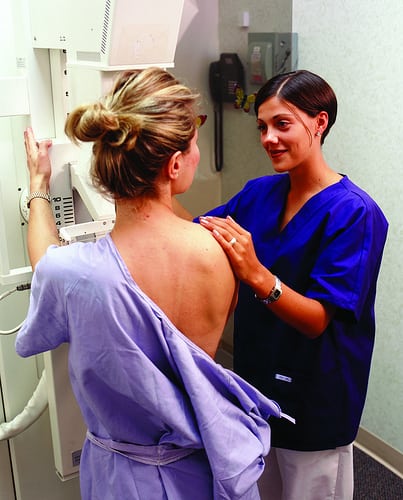
Mammography involves taking multiple X-rays of the breast tissue using “low-dose” ionizing radiation in an attempt to detect cancer. During the process, a woman’s breast tissue is compressed to get a clearer picture. A “screening mammogram” is often followed by a “diagnostic mammogram” if the radiologist sees any suspicious findings.
How Accurate Are Mammograms?
Dense tissue, like that typically found in women under 50 years old, is notorious for producing false negatives and positives. The false positives result in anxiety, more mammograms, and often painful surgical procedures. In 2009, the U.S. Preventive Services Task Force recommended mammography every 2 years for most women from the ages of 50-74 to reduce the incidence of anxiety, unnecessary surgery, and the small but real possibility of breast cancer induced by excess radiation from the mammograms themselves. They concluded that the evidence did not substantiate routine mammograms in women under 50 or over 74. The recommendations mean a woman would undergo just 13 mammograms by 75, rather than the 35 she would experience if she began annual testing at age 40. This created an uproar among many mainstream doctors and cancer organizations like the American Cancer Society (ACS) and the National Cancer Institute (NCI), who were recommending mammograms starting at age 40. They claimed that such messages were putting women’s lives at risk.
In 2011, a study concluded that mammograms reduce mortality from breast cancer by an absolute amount of only 0.05%. According to their analysis, 1 in 2,000 women will have their life prolonged by 10 years of screening; however, another 10 healthy women will undergo unnecessary breast cancer treatment. Additionally, 200 women will suffer from significant psychological stress due to false positive results. They questioned whether mammography screening does more good or harm and stated that universal screening may not be reasonable. I’m sure you can guess the reaction from the ACS & NCI.
How Safe Are Mammograms?
If cancer is already present, the compression from the procedure can rupture vessels and cause the cancer cells to spread. Doctors used to be instructed to avoid over-manipulating suspected tumors to avoid this possibility, but somehow, this advice doesn’t apply to mammography. The amount of radiation to one of the most sensitive tissues in the body can also be substantial. Research shows that a single mammography screening can produce the equivalent amount of radiation in 1000 chest X-rays.
Are They Saving Lives?
Women whose breast cancer was detected by screening mammography before the appearance of a lump or other symptoms commonly assume that the mammogram saved their lives. Most cancers found by mammography fall into 1 of 3 categories:
1. Cancers that are not very aggressive and later detection would have resulted in the same outcome.
2. Cancers that are so aggressive that even “early” detection doesn’t save her life.
3. Cancers that would have receded on their own or are so slow-growing that the woman would die of other causes before the cancer produces symptoms. Ductal carcinoma in situ (DCIS) is now being seen and diagnosed as early-stage breast cancer in women (stage 0). DCIS is, in fact, not cancer and simply a calcification of the milk ducts that often does not progress to cancer. A diagnosis of DCIS often leads to unnecessary invasive treatments. This is skewing the cancer survival rates as these women as being counted among the “survivors” of breast cancer and used by cancer societies as “proof” that screening works.
That being said, there are a small number of breast cancers that are detected by screening mammography and whose treatment outcome improves as a result of earlier detection. Data suggests that between 3-13% of breast cancers fall into this category. In other words, mammography does not benefit any of the remaining 87% to 97% of women. Can we do better?
Are There Alternatives?
MRIs are one option that doesn’t involve ionizing radiation; however, these are not practical for large-scale screening due to the high costs involved. Thermography, on the other hand, involves thermal imaging, is a great option that doesn’t involve ionizing radiation or compression and can detect abnormalities years before mammography. Also, unlike mammograms, breast tissue density and surgical implants don’t affect the ability to interpret the scan. Unfortunately, because this imaging isn’t covered by insurance, few women hear about or seek out what many, including myself, consider a superior imaging option. The cost is typically a few hundred dollars.
So why was I so upset about what had been done to my mom? Let’s put the stupidity of the tech’s comments aside and talk about the procedures performed. The mammogram was, in my opinion, completely unnecessary. An ultrasound could have been performed from the start, particularly since she already knew exactly where the lump was located, and a skilled technician could view other areas of the breast for possible tumors. Ultrasound does not emit ionizing radiation or compress the breasts, which can potentially spread cancerous cells from an existing tumor.
Additionally, an ultra-sound is more specific when deciphering between a solid mass (more suspicious of cancer) versus a fluid-filled mass (more likely a benign cyst). I understand that mammograms are the standard of care; however, I want to see that change. Women should know that they have options and shouldn’t let their health care be dictated and limited by an insurance company.






Back in Spring 1990 at the age of 35 I asked for a screening mammogram due to a high family history of cancers. Late fall I found a moderate size lump, was told “it’s probably a cyst, use a warm washcloth”. It started to ache in the area, so now I am told “cancer doesn’t hurt” but I decided action was required. Doctor’s eyes got really wide when he palpated it, got my “Christmas Mammogram”, needed “more views” and got my “New Year’s Mammogram”. One afternoon I unloaded a pickup truck of hay (common chore) and the lump more than doubled in size, sticking out like the corner of a box! Boy howdy, did that ever scare me to death! Long story short, Modified radical Mastectomy at age 36, simple on the other side and bilateral reconstruction the following year. The mammogram didn’t turn up anything, the only real good is that nobody could look at me and say it (tumor) “had been there for years”.
Funny thing is, I have to fight to NOT get mammography now, even though there is no breast tissue requiring compression!! Any way, I’m now “20, almost 21 years old” and just got my third set of implants- who knew they actually expect them to need replacing regularly?? Self exams, ladies! Safest and best track record!!!
Amen! Amen! and Amen! I have been saying this for years, literally! My husband was a medical device product safety engineer with a very large product safety company (a direct competitor of United Labs) and he has always said that mammograms are the worst type of diagnostic tool. I am only 36, but I decided years ago to never have a mammogram. Why would I when there are other, better diagnostic tools out there. I have stated this to different primary care physicians I’ve had over the years and they definitely do not like to hear it. But, unless a change is made w/in the insurance companies, I will pay for my own preferred method of diagnostics myself, if I feel it is necessary and not because I’ve hit an arbitrary age.
p.s. CT Scans are just as dangerous!
Thank you for this article! Even as I read this, my mom (a *real* 🙂 breast cancer survivor), is having surgery to remove a kidney that was found to have a tumor and spread to the breasts and lungs. This time, the cancer is stage IV and unrelated to her previous breast cancer. We have been told that the breast cancer is genetic, my mom having been the 4th generation in which it has appeared. Anyway, all that to say that I was unaware of alternatives mammograms and all that, and have myself all worked up for the time when those tests need to be done, still many years off. The medical community will immediately “red-flag” me because of my family history, so I am appreciative of this information that there are options for less invasive and more accurate testing. Thank you!
[…] Mammograms: Helpful or Harmful? : Modern Alternative Health […]
[…] – Mammograms: Helpful or […]
It is illegal for a tech to give results or ask about treatment. They can be punished and have action taken against their license for something like that….Those results are only allowed to be given by a doctor.
I have a 2nd cousin, a grandmother, and an aunt, all blood relatives on my mom’s side, who had breast cancer. My 2nd cousin’s was a very aggressive Stage 4, found solely on mammogram (no other symptoms and no lumps on her BSE); she elected to participate in a chemo research drug trial… she is currently in remission and doing very well. My aunt and grandmother had it, both died from metastasis to the brain, bones, and lungs. My aunt had a false negative biopsy when she first went to the doctor about a lump. By the time they realized it was really cancer, it was too late. My grandmother apparently had all the signs of breast cancer, but never told anyone (she revealed this info on her death bed). This was back in the early 1980’s and my mom has always said that she wished mammograms were common place then and maybe the outcomes would have been different. Who knows. My mom, my sister and myself are all considered genetically high risk and are supposed to get mamms every year. I also do my monthly BSE and visit my GYN yearly for a well woman exam. Based on my family history, I do get and WILL continue to get mammograms, but am torn on whether to go every year or every 2 years. My insurance covers preventive screenings 100%, so cost is not an issue at all, the place I go is 5 minutes down the road and they have a dedicated room just for system employees so we can walk right in without an appointment. I am overweight but otherwise healthy (no chronic health problems, rarely take medications, no food allergies, etc.). Maybe I’ll go every 2 years until 50, then every year? But my aunt died at 38… feel my dilemma?
Dr. Perez notes that, “The amount of radiation to one of the most sensitive tissues in the body can also be substantial.” Yes, and a most accurate understanding of this is that any dose of a x-ray is “substantial” because it was found the the lowest dose of ionizing radiation is carcinogenic (discussed in Rolf Hefti’s ‘The Mammogram Myth’ – more at TheMammogramMyth dot com). Yet this solid knowledge has been (1) twisted by the medical industry claiming it is an inconsequential danger, and so (2) it hasn’t stopped the enormously large medical business from using these very harmful procedures, having cost the lives of millions of unwitting people.
[…] Mammograms: Helpful or Harmful? […]