Image by grendellion
Unfortunately, labor and birth (and pregnancy) don’t always proceed smoothly. Sometimes situations that warrant interventions do arise. And sometimes those situations are emergencies that require immediate action. What happens to your rights when things go wrong? What can you expect, or should you expect?
When Things Go Wrong (Non-Emergency)
Most situations where things begin to wrong are not immediate emergencies. For example, one of the common “red flags” is baby’s heartrate dropping during contractions and not recovering like it should. This is definitely something that warrants attention, but not an immediate we-must-do-something-now emergency.
In a situation where something may be happening, you should be offered an explanation of what’s happening, as well as a series of options for treatment. This may need to be explained quickly, but you have a right to know. In the decelerating heartrate example, you may be asked to change positions (this sometimes fixes it), have medications changed, be given something to augment labor, or — if nothing else is working there is a serious concern about how baby is tolerating labor — given a c-section.
Ask what all the options are and that they be explained to you, and ideally, if it isn’t an immediately serious situation, try the least intervention first to see if it will help.
Remember that you have a right to:
- Know what the situation is
- Know why doctors are concerned (what the possible negative outcome could be, without the scare tactics)
- Know what all the possible treatment options are
- Know the risks/benefits of these options
- Know the risks/benefits of doing nothing (although you won’t usually want to do this in a situation where something’s wrong)
Ask, if it is not explained to you. In “something’s going wrong” non-emergency situations, they usually have five minutes to explain things to you before making a decision.
When An Emergency Occurs
Sometimes, though, something happens that is a true emergency. A we-must-intervene-immediately-or-else kind of emergency. Cord prolapse is usually such an emergency. Uterine rupture is such an emergency.
In these cases there are usually no options and no time to explain very much. For very serious situations, a c-section is usually the best, if not only, course of action. Be aware of that.
As you are being prepped for immediate intervention though (this will still take a couple of minutes), you have the right:
- To hear, briefly, what has happened (i.e. “We have a cord prolapse situation here, which could cause your baby to lose oxygen, leading to brain damage or death”)
- To hear what is being done to you now (i.e. “We need to perform an emergency c-section to save you and/or your baby’s life”)
- To keep your support person/people with you if at all possible
- To be talked through the procedure by a nurse or other medical professional (i.e. “We’re prepping you for surgery now…your baby will be out in just a minute…”)
- To ask to see/hold your baby immediately, unless s/he needs medical attention
- To be given a de-briefing after the event
The de-briefing occurs after you and baby are both stable and in recovery. The doctor should come and explain to you what happened, why they performed the intervention they did, and mention anything that you ought to know about recovery, what to expect in you and baby, signs of complications (like infections), etc. This is also your chance to ask any questions that you have.
Sometimes things happen quickly out of necessity, but you always have the right to as much information as there is time to give — at a minimum, “This is what happened and this is what we are doing now.” You also have the right after the fact, when everyone is stable, to have all your additional questions answered. Compassionate doctors will come as a matter of course to talk to you after something goes wrong.
What if it Wasn’t a Real Emergency?
In very rare cases, doctors say it is an emergency when it is not. There have been a few reported cases of women being “tricked” into c-sections (usually mamas who are there for a VBAC) and who are never given informed consent.
There is not a lot that you can do in these cases. Request your medical records, report the doctor to the medical board, consult a lawyer well-versed in medical law. Unfortunately, if this does occur, medical records may be falsified or doctors may have even obtained a court order declaring a woman incompetent, so they are legally protected. It’s highly unethical…but there’s little you can do.
Be assured these situations are very very rare, I only mention them because they have happened a few times. Making sure you feel comfortable with your provider and asking all your questions during prenatal visit should help prevent anything like this from happening.

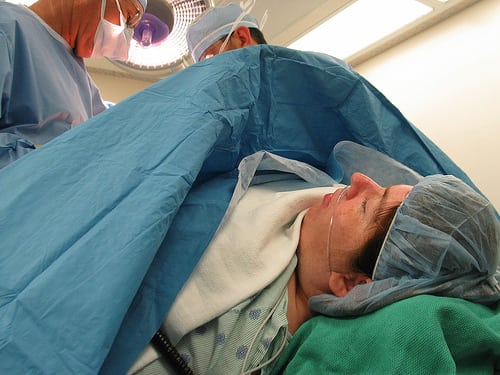



I faced a semi-emergency at home…baby was in distress as she spent two hours in the birth canal because I was too exhausted to push effectively. By the time it was clearly an emergency, we were running out of time to transport. My midwife reluctantly performed the second episiotomy of her career (the other was an 11 lb baby!) and essentially yanked the baby out. She had to have oxygen, but recovered from the birth stress by the end of her first day.
My midwife did not ask my permission or my husband’s to perform the episiotomy. I was not lucid during the last 15 minutes of labour and did not understand the situation (in fact. I kept trying to push after baby was out!) and my wonderful, supportive husband was very afraid for us and beginning to lose his grip. I didn’t know I’d had an episiotomy until it was time to sew up (I thought I had torn). Am I okay with this? Definitely. I believe my midwife’s willingness to do it despite her strong belief in the natural process may have saved my baby’s life, or at least health.
Interesting note: If I had been in the hospital I almost certainly would have had a c-section and had that happened, I probably would have considered it a necessary c-section. However, since I didn’t have one and ended up with a healthy baby and a good postpartum recovery, I clearly didn’t need a c-section…so I’m also very grateful that we were at home. My mother reminded me several times during recovery that ‘It’s much better to be recovering from a home epistiotomy than a hospital c-section!’ Yes, it certainly was!
Oh, and let me add that while I was thankful for the emergency intervention, I am pregnant again and will be discussing how to prevent the emergency from ocurring in the first place this time at my next prenatal!
It makes me so sad when I hear stories of those emergencies that weren’t really emergencies that lead to unsatisfying deliveries. Like you say, there’s really not much that you can do about it once it’s done. That is what makes it so incredibly important to select a birth team that you fully trust long before it comes to that point.