Most women give birth in the hospital. That’s the current trend in the U.S. and many women feel safer in the hospital, for one reason or another. Some women, those who are high-risk, may need to be in the hospital in order to give birth safely. Regardless, the women who birth in hospitals face special issues with informed consent: do you have to ‘consent’ to every procedure? If so, how? If not, why not?
Many women are under the (unwitting) delusion that once you are in a hospital, that you must submit to whatever procedures they recommend. This is usually not true, but it also depends on the pre-admit forms that you sign. Typically, though, you have the right to refuse any treatment that you do not want. Remember that.
What is Informed Consent?
Informed consent is the idea that you must be fully aware of the risks and benefits of a procedure, as well as other options in your situation, before agreeing to undergo that procedure. A doctor should provide you with:
- A diagnosis or description of the situation, if possible
- His/her recommended procedure or treatment
- The full risks and benefits to this procedure or treatment
- Alternative treatment options — anything available, regardless of cost or insurance coverage
- The risks and benefits of alternative options
- The risks and benefits of refusing all treatment
If your doctor does not provide you with this full set of information, and treats you anyway, or bullies you into saying “yes” (which is ‘consent’ but not ‘informed consent’), s/he may be charged with battery or negligence and may face a malpractice lawsuit. Pay attention to that last part: even if you say yes, the doctor may still face disciplinary action or legal charges if the consent was not informed.
Many women these days are bullied into accepting procedures that are not always medically necessary. Often times these procedures or medications are administered by the nursing staff, without any contact with a doctor. This is illegal.
The prescribing doctor must come in him or herself and explain to you the treatment that is recommended and obtain your informed consent.
Why This Matters
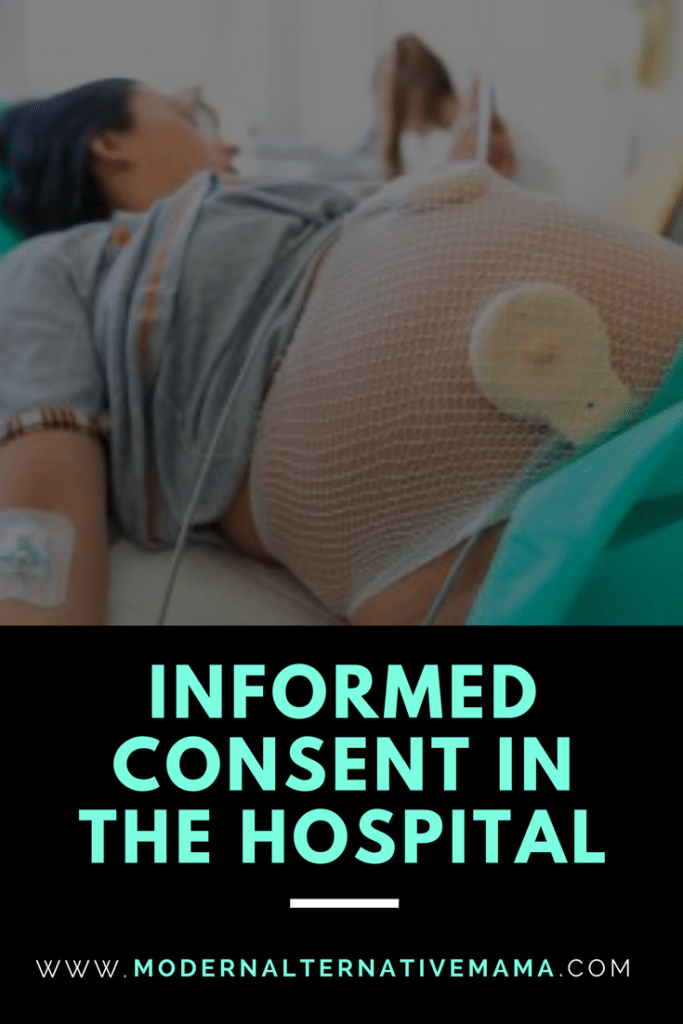
Women are simply being told what to do during birth, many times. When a woman arrives at the hospital, she is often told “We’re starting an IV now.” If her labor isn’t progressing fast enough according to the hospital’s timeline, she may be told, “We’re starting Pitocin.” These statements are made, there is no question asked — “Our usual procedure is to start an IV line. Are you okay with that?” And there is no additional information on the risks and benefits provided.
Women often feel bullied and pressured into accepting treatments that are not medically necessary. Interventions in labor are often a cascade effect. A woman has an IV started and continuous fetal monitoring “because that’s what we do,” so she is confined to a bed for the most part. She struggles to cope with the pain when she has to remain still and on her back, so she opts for an epidural. This slows her labor, so the staff announces “We’re starting Pitocin.” Her labor still doesn’t progress, and she ends up with a medically unnecessary c-section.
There are several different ways this situation can happen besides this example, but the trend is the same: the hospital staff begins their “normal procedures” and women, feeling that they have no choice but to submit, do so and end up with a very different birth than they had anticipated — and not due to any medical necessity.
You Do Have a Choice
Even when you sign the pre-admit forms, which gives the hospital permission to treat you, it does not remove the physician’s duty to provide informed consent for each procedure that s/he would like to perform.
If someone comes into your room and announces “We are doing this now,” you do not have to allow them to. Instead, you might say:
- Who has ordered this? Was it my doctor?
- Can I speak to the doctor who ordered this procedure?
- Is this procedure medically necessary at this time?
- What are the risks and benefits of this procedure?
- Are there alternatives?
- What risks and benefits are involved in having no treatment at this time?
If you are not satisfied with the answers, you have the right to ask for a second opinion…or to simply say, “No, I do not consent to that.” Be clear. Don’t say “I don’t really want that,” or “I don’t like that idea.” Say, “I do not consent.”
Unfortunately, the staff may become upset with you. They may roll their eyes, sigh, or say, “I’ll have to call the doctor and see if he’ll allow that.” They may try to say, “We have to, it’s hospital policy.” But you never have to consent to a non-emergency procedure that you do not want. Do not let them lie to you or bully you.
A good doula and/or other support may come in handy here. When in labor, you’re not in a frame of mind to stand up for yourself and to argue with those around you. Your support people can fill this role for you. Make sure that your support people are aware before you enter the hospital what you will and will not consent to (given a non-emergency situation).
Evidence-Based Medicine
This is a phrase that a lot of doctors throw around when advocating for hospital births, c-sections, and other medical interventions. Although this is sometimes necessary, it is also performed more than needed.
You have the right, as a patient, to ask for evidence-based practice. “You’ve been in labor for 8 hours now,” is not an evidence-based reason for starting Pitocin, if you and baby are tolerating labor well. That would be for convenience of the doctor and/or hospital staff, or because it is considered “procedure.” This is not good enough and you do not have to submit to something just because it is “procedure.”
Throughout this month, we’ll be talking about more issues you may face with informed consent: doulas, midwives, newborn procedures, and lots more. We’ll talk about how to handle it when someone does try to bully you or talk you into procedures without medical evidence.





Sadly I see things like this a lot as a doula. For instance a mom agrees to get checked to see how far along she is and I see the OB hold out his hand and the nurse hand him an amnio-hook. All somehow without words. I am glad I am there to jump in and say, “It looks like the Doctor is going to break your water, do you have any questions you want to ask before agreeing to that?” This is just one of many examples.
I really wish that they would always explain and ask! It is frustrating that they don’t.
Thank you, thank you, thank you! This is exactly the information that I’ve been needing. I’m really curious if having a iv during labor is necessary. Can I decline that? Thank you for this information!
This is such a good post! With my first baby, I was told what to do through the entire labor and delivery, and never given an alternative or even asked. IV was mandatory I was told – for what? They gave me drugs without my consent that caused me not to have any memory or consciousness for nearly 24 hours, and an epidural while under those drugs that I also did not consent to. This resulted in all types of complications and me pushing for over 4 hours. I was told that these were “hospital procedures” and for my benefit. Never again, I said! I went to a midwife for my next 2 and totally unmedicated – the result was both of them being born within 2 hours of my arrival, pushing for 45 minutes with 1 and 15 minutes with the other. Natural makes so much more sense! And if medicine is necessary, it only makes sense to explain why and how it will affect me. I mean, I am the one who must live with the side effects they cause, right? I do not understand why some hospital staff is so against allowing patients to make informed decisions. And after having that horrible first birth and fighting with staff every step of the way for 2 natural births, I am thankful to be going to a birthing center this time around and having every decision made by me and my husband. My requests are being respected and listened to. What a concept!
this reminds me of my labor, delivery, recovery process w/ my 1st. (currently working on the 2nd due in DEC. 2012).
anyhow. the nurses & doctor were mostly satisfactorily informative well enough throughout the labor & delivery.
in the recovery room, though, a nurse hooked my I.V. to a bag of something & I saw that it was pitosin. I told her I didn’t want pitosin & she, “snottily” (instead of apologizing or being understanding) told me I needed it (I had an emergency c-section), that the pitosin would help contractions “shrink” my belly & this was vital for my health. & quite said that it was dangerous for my health NOT to have the pitosin. I believed her well enough, my baby was out, so baby wouldn’t be suffering the effects. & it was a low dose apparently.
the problem was, she didn’t say anything before just giving me a synthetic hormone. I asked what side effects there might be, & she said there’s no side effects. OK…? I had this nurse for a while at the beginning of my recovery & she either didn’t know anything or didn’t care or was just insensitive or a combo. but she seemed to think that none of the drugs had any side effects when I would ask.
I realize that a lot of people have very negative experiences to share and have been very hurt by what they have experienced, but I thought I would share one of my experiences that was very positive…there are some WONDERFUL care providers out there! I was induced at almost 42 weeks with my first. I had not dilated at all and was barely effaced. We were confident of dates as I had been charting before getting pregnant and had numerous conversations with our midwife about induction before finally deciding to go ahead with it. I was planning to have a birth without pain meds. Shortly after labor began with pitocin, my son’s heart rate started dropping with each contraction. It recovered well between contractions and our nurse and our midwife kept encouraging us to keep pressing ahead. I was dilating very slowly and had all back labor. My midwife felt that our son wasn’t in a very good position and gave me lots of things to try to get him into a better position. The positions I tried to labor in led to even greater drops in heart rate for our son. Our bodies were just not working together. Around midnight, I ended up getting an epidural because the position that was best for my son was laying on my back/slightly on my side and I couldn’t manage the pain that way. As time went on, my son’s heart rate was taking greater dips and remaining low for longer periods of time. I knew that I was likely headed for a c-section, but my midwife and my nurse kept encouraging us. My nurse even prayed with us and recited scripture to us. I can still remember so clearly how at 3:45am my midwife came in and sat on the edge of my bed. She expressed her concern with how things were going and recommended an emergency c-section. She went through everything with us – risks/benefits, recovery, health of the baby, future deliveries, choices we could make. At the end of the conversation, she left it with “My recommendation is that we get your baby out of you as quickly as we can, but that decision is ultimately up to you.” We decided to go ahead with the c/s. Our little guy was born at 4:46am. The cord was wrapped tightly around his neck, but he was healthy. The OB who got out of bed in the middle of the night to deliver our son was fantastic. He complimented us for how hard we tried to have our son naturally and counseled us that things don’t always work out the way we planned and even encouraged us that a VBAC would be an option the next time around. Our midwife stayed with us for the surgery and assisted the OB. Obviously, this is not how we would have liked everything to have gone down, but it did and we will forever be thankful for the wonderful care we received in the process. I had a successful, pain med free (although induced) VBAC 20 months later. And, now I am at 37 weeks with #3 hoping for another successful VBAC and PRAYING that I go into labor on my own! It’s so easy to get frustrated with the medical professionals available to us for our care. But, one of the best things about our nation’s healthcare is that we have the choice of who will deliver our babies and where they will be delivered. We need to be willing to ask questions from the earliest prenatal appointments and keep those conversations going with our care providers and change providers as soon as we feel that they have anything other than our best interest in mind. We can’t place all the blame and responsibility on them – we need to be educated and knowledgable.
Love this new site – but you need some share buttons on the posts! 😉
Great info, thank you. Can you post about those of us who test positive for group b strep? What are our alternatives? What are the risks (to the baby) if we have or do not have the antibiotics?
THANK YOU!
I gave birth at home, but I have heard that a lot of hospitals and doctors will sneak a waiver of informed consent into your check in paperwork. Be careful what you sign in the rush!
I wish I had seen an article like this before my son’s birth. My (former) doctor made it sound like a he was super pro-natural childbirth until I checked into the hospital. Then everything changed. There were many unnecessary procedures done without informed consent, including the start of pit immediately after he was born. The ones that I attempted to refuse resulted in bullying and threats to remove me from the hospital because I was going against their routine procedure. The doctor said he would refuse to see me if I insisted on being able to walk and because I wanted a hep-lock rather than an IV. He kept threatening me with an internal monitor if I didn’t sit still and said I needed to get the baby out by 8pm because he had somewhere he needed to be. My personal experience in a hospital was absolutely horrible. I know it isn’t for everyone but I have such distrust of doctors now. I hope to have a home birth if I’m ever blessed with another baby.
Thank you for this post and for putting this information out there for women.
[…] by immediate delivery for fetal distress).